Bacteria samples from all over the globe found to have antibiotic resistance genes, says research
02/22/2019 / By Michelle Simmons
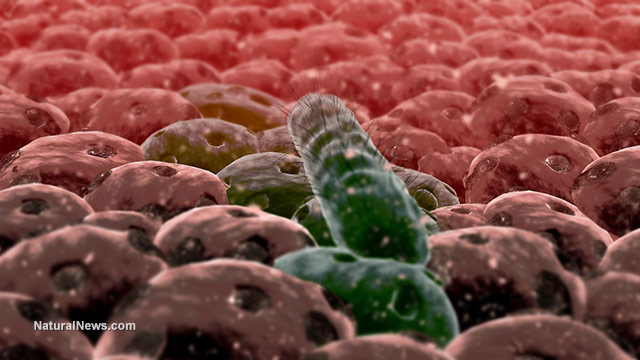
Researchers warn that infections caused by antibiotic-resistant bacteria will continue to increase each year, especially since these acquire more resistance genes from other bacteria. The effects of such a genetic delineation prompted scientists from the Chalmers University of Technology and the University of Gothenburg in Sweden to evaluate large numbers of bacterial DNA. Their study looked at DNA sequences of bacterial samples from people and environments from all over the globe.
The results of their study, published in the journal Microbiome, concluded that there are at least 76 new types of antibiotic-resistant genes, several of which can give bacteria the ability to degrade carbapenems, the most powerful class of antibiotics used against multidrug-resistant bacteria.
“Our study shows that there are lots of unknown resistance genes. Knowledge about these genes makes it possible to more effectively find and hopefully tackle new forms of multi-resistant bacteria,” said Erik Kristiansson, lead investigator of the study and a professor at Chalmers.
He added that identifying a resistance gene is difficult, especially if it has not been known in the past. To identify a resistance gene, Kristiansson and his team developed a new computational method to determine patterns in DNA that are linked with antibiotic resistance. Then, they tested the genes they identified in the laboratory to confirm their predictions.
“Our methods are very efficient and can search for the specific patterns of novel resistance genes in large volumes of DNA sequence data,” said Fanny Berglund, one of the researchers of the study.
The researchers plan to identify the genes that influence the resistance of bacteria to other forms of antibiotics. Kristiansson said that the novel genes that they found are “only the tip of the iceberg” and there a still a lot of unknown antibiotic-resistant genes that could lead to major global health problems in the future.
The threat of antibiotic-resistant bacteria worldwide
People have treated antibiotics as the silver bullet when it comes to treating infections since the 1940s. Yet, recent studies show that bacteria have become antibiotic-resistant: These strains can cause infections that are harder to treat compared to non-resistant bacteria.
This is one of the biggest threats to global health, food security, and development today, according to the World Health Organization. Ever year, drug-resistant infections end the lives of at least 700,000 people. If not acted on immediately, this number is expected to increase tenfold by 2050. Drug-resistant infections not only lead to increased deaths, but also higher medical costs, and longer stays in the hospital. One of the primary causes of antibiotic resistance is the overuse of antibiotics to treat conditions that do not require antibiotics. Misuse of antibiotics is also common in agriculture, where at least 240 million kilograms of antibiotics are used in livestock every year. (Related: Antibiotic-resistant bacteria found in hospitals likely came from industrial livestock farms.)
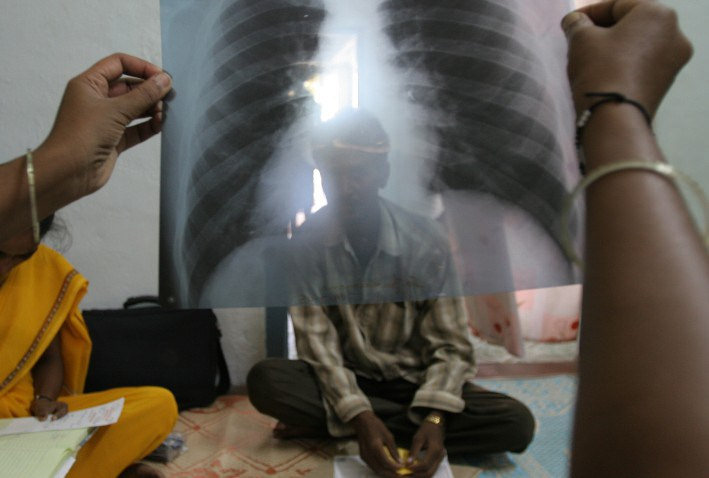
Infections, such as pneumonia, tuberculosis, blood poisoning, gonorrhea, and foodborne disease, are continually becoming more difficult or impossible to treat because antibiotics are becoming less effective. According to the Centers for Disease Control and Prevention, every year in the U.S., at least 2 million people are infected with antibiotic-resistant bacteria, with over 23,000 dying as a direct consequence of these infections. Some of the bacteria resistant to medications are methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococcus (VRE), multi-drug-resistant Mycobacterium tuberculosis (MDR-TB), and carbapenem-resistant Enterobacteriaceae (CRE) gut bacteria.
Find out more scientific breakthroughs at Research.news.
Sources include:
Tagged Under: antibiotic-resistant bacteria, Antibiotics, bacteria, biomedical research, infections